|
Nonverbal evidence of pain may or may not be congruent with verbal reports, thus indicating the need for further evaluation. 
Note the presence of behaviors associated with pain- changes in vital signs, crying, grimacing, sleep disturbances, withdrawal, or narrowed focus Pain may be localized to the chest wall or referred to the ipsilateral shoulder or upper abdomen because of diaphragmatic irritation. It is typically described as sharp or stabbing and is exacerbated with deep inspiration. Pain assessment helps determine the choice of interventions and provides a basis for comparison and evaluation of therapy. The client may also have a high or low tolerance to pain and pain medications.Īssess pain comprehensively, noting location, duration, precipitating and aggravating factors, and severity using a 0 to 10 scale. The perception of pain can be influenced by age and developmental stage, underlying problems, and cognitive, behavioral, and sociocultural factors. Demonstrate the use of therapeutic interventions to minimize pain.Īssess the client’s perceptions of pain and attitude toward pain.Verbalizations of pain aggravated by coughing or breathingĪfter the implementation of nursing interventions, the client is expected to:.The pain may diminish in intensity as the pleural effusion increases in size and the inflamed pleural surfaces are no longer in contact with each other. The presence of chest pain, which results from pleural irritation, raises the likelihood of an exudative etiology, such as pleural infection, mesothelioma, or pulmonary infection. The following are nursing diagnoses associated with pleural effusion.īelow are sample nursing care plans for the problems identified above. Nursing interventions for a client diagnosed with pleural effusion include determining the etiology of the pleural effusion and addressing the underlying cause. If pleural effusion is mainly due to these mechanisms, then increased hydrostatic pressure usually causes transudative, leading to pleural effusion that has an altered balance between hydrostatic and oncotic pressures (usually transudates), increased mesothelial and capillary permeability (usually exudates), or impaired lymphatic drainage. Accumulation of excess fluid can occur if there is excessive production or decreased absorption or both overwhelming the normal homeostatic mechanism. Hydrostatic pressure from the systemic vessels that supply the parietal pleura is thought to drive the interstitial fluid into the pleural space and hence has a lower protein content than serum. Pleural fluid originates from the vasculature of parietal pleura surfaces and is absorbed back by lymphatics in the dependent diaphragmatic and mediastinal surfaces of the parietal pleura. Common causes of exudates include pulmonary infections like pneumonia or tuberculosis, malignancy, inflammatory disorders like pancreatitis, lupus, rheumatoid arthritis, post-cardiac injury syndrome, chylothorax (due to lymphatic obstruction), hemothorax, and benign asbestos pleural effusion. Pleural fluid LDH is more than two-thirds of the upper limits of normal laboratory value for serum LDH.Ĭommon causes of transudates include conditions that alter the hydrostatic or oncotic pressures in the pleural space like congestive left heart failure, nephrotic syndrome, liver cirrhosis, hypoalbuminemia leading to malnutrition, and the initiation of peritoneal dialysis.The pleural fluid lactate dehydrogenase (LDH)/serum LDH ratio is more than 0.6.The pleural fluid protein/serum protein ratio is more than 0.5.Pleural fluid is considered an exudative effusion if at least one of the criteria is met. 
Pleural fluid is classified as a transudate or exudate based on modified Light criteria. Pleural effusion is one of the major causes of pulmonary mortality and morbidity. It can occur by itself or can be the result of surrounding parenchymal diseases like infection, malignancy, or inflammatory condition. Morbidity and mortality rates of pleural effusions are directly related to the cause of the underlying disease at the time of presentation, as well as biochemical findings in the pleural fluid.Ī pleural effusion is a collection of fluid abnormally present in the pleural space, usually resulting from excess fluid production and/or decreased lymphatic absorption. Pleural effusion is the most common manifestation of pleural disease, and its etiologies range in the spectrum from cardiopulmonary disorders and/or systemic inflammatory conditions to malignancy.  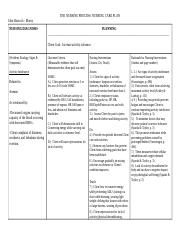
Approximately, 1.5 million pleural effusions are diagnosed in the United States each year.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
